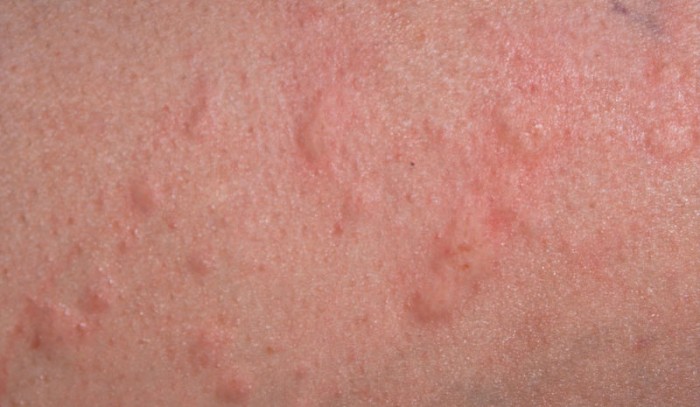
Also known as ‘nettle rash’ or hives, urticaria is a form of skin rash. It generally takes the form of raised wheals or welts on the skin which can be itchy or even cause a stinging or burning sensation. Whilst frequently caused by an allergic reaction this is not always the case; as a rule short term (acute) episodes of hives tend to be caused by an allergy whereas those that last longer than six weeks (chronic) are rarely due to allergies.
Hives are one of the most common skin conditions, affecting around 20% of people at some point in their lives. In most cases this does not cause much more than an annoying distraction which passes quickly with the cause never being identified. And whilst allergies are a factor in many cases other triggers such as stress, overheating, exercise, illness, or even alcohol can all be responsible.
Unlike other allergic skin conditions such as allergic contact dermatitis, urticaria is often an immediate response to an allergenic substance.
Sometimes the same type of reaction responsible for causing hives occurs at a deeper level of the skin causing swelling. This is known angio-oedema, and although usually not itchy it can be painful. Unlike urticaria, which is as likely to appear anywhere on the body, angioedema is more common on the face and even the tongue causing significant discomfort.
Symptoms of Hives
The symptoms of hives may last a matter of minutes (acute) or several months (chronic). For those familiar with nettle stings, hives are similar in appearance.
- Raised bumps (weals) which can be fairly pale through to red. When pressed they will “blanch”, i.e. turn white. These bumps are often clear around the edges.
- Redness and itching of affected area of the skin.
- Hives may appear rapidly on any part of the body – and disappear just as quickly.
The main symptoms of angioedema include:
- Swelling, most commonly affecting the skin of the arms, legs, torso or face. Lips and tongue are common sites.
- Complications include swelling of the upper respiratory tract which may interfere with breathing. There can also be swelling of the lining of the eyes (chemosis)
Causes of Hives
It is no coincidence that hives is also known as nettle rash. Nettle stings are delivered via tiny glass hairs on the plant which contain histamine, the main chemical involved in allergic responses. The result is the appearance of small, raised wheals and redness of the surface of the skin.
Histamine is part of the body’s inflammatory responses and is released locally when the body believes it is under attack. Its role is to make the blood vessels more leaky allowing the release of infection fighting white blood cells. In an allergic reaction the body mistakes a usually inoffensive substance as an attacker.
There are a range of factors that can cause hives:
- Direct contact with the allergy causing substance. This can be a range of allergens from food additives to other common triggers.
- Physical stimuli such as heat, cold, pressure, exercise or even sunlight.
- Infections and medical conditions, e.g. thyroid disease, urticarial vasculitis, erythema multiformae or Stevens Johnson Syndrome.
It is also worth noting that urticaria is also one of the early symptoms in nearly all serious allergic reactions.
Diagnosis of Urticaria
Unfortunately the cause of most long term cases of urticaria remains unknown (idiopathic). Skin prick test rarely reveal the culprit and the most effective tests are elimination diets with specific allergen testing.
Sometimes acute urticaria can be easily recognised as the reaction occurs immediately after exposure to the allergen, such as a food or medicine.
It is also important to rule out any underlying conditions in cases of long term urticaria.
Urticaria Treatment and Management
The best strategy for dealing with hives depends on the cause. Whilst to many this remains unknown, the good news is hives often clears up without any treatment.
Obviously, if the trigger for your urticaria is known then the best way to manage the symptoms is to avoid the cause. For the rest of those suffering hives there are effective treatments to reduce the discomfort.
For most cases antihistamines will be the most effective medication. Generally available over the counter these work by blocking the main antagonist in hives, the messenger chemical histamine. These are usually effective in reducing the itching and hives within around 30 minutes and can provide long lasting (24 hour) relief. Antihistamines also have a preventive role in that they can prevent an episode of urticaria occurring before it does.
Antihistamines have improved greatly over the years and the latest generation are far less likely to cause the drowsiness that was associated with older ones. Newer, reputedly non-sedating antihistamines include Allegra, Zyrtec, and Claritin and their generic versions. However, it is often a case of trial and error finding a medication that suits you and many find the older, first generation antihistamines equally effective, as well as being far cheaper.
For more severe episodes of urticaria some form of corticosteroid or immune modulator may be prescribed to control the symptoms.
In addition to medicines there are some simple ways to manage urticaria which apply to all forms. These include avoiding:
- Scratching or excessive rubbing. This is a common cause of physical urticaria and exacerbates other forms.
- Tight or constrictive clothing. Looser fitting clothing and no restrictive belts are the way to go.
- Sun exposure. Sunlight can trigger various forms of hives.
- Extreme temperatures, or changes in temperature. Both cold air or getting too hot can be a trigger.
Self management of hives is sufficient for the vast majority of cases. However, if your symptoms are severe or last longer than 6 months it is always worth visiting your doctor.